How to prevent getting the flu during coronavirus:
Learn the difference and similarities between the flu (Influenza) and coronavirus (COVID-19)
Written by Dr. Ruby Rose, MD.
We are all adapting to our new normals, both at home and at work. We at SignatureCare Emergency Center understand the struggles of staying safe while living an active and productive life. We hope this article helps prepare you for the upcoming flu season in the age of COVID-19.
As we surpass the US death toll of over 200,000 COVID-19 deaths, one cannot fathom how this could get worse. The CDC has estimated that the annual deaths due to the influenza virus since 2010 are between 12,000 to 61,000, with hospitalizations reaching over 800,000. Now imagine this number with COVID-19 as an additional threat.
While most patients who contract influenza or SARS-COV-2 (the virus that causes COVID-19) will recover without serious complications, some can progress to serious illness, hospitalization, and death.
Furthermore, we are discovering more residual complications from the SARS-COV-2 virus. There is still a lot of data we do not know about this novel virus. What we do know is how to prevent contracting the flu and along with that reducing our exposure to coronavirus.
Influenza and coronavirus: What’s the difference?
Influenza (the flu) and coronavirus are both contagious respiratory viruses. Table 1 (below) displays the similarities and differences between the two viruses. Both viruses cause similar symptoms. However, the coronavirus can cause additional symptoms that are specific to the SARS-COV-2 virus such as the loss of taste and smell, among others.
Coronavirus has also proven to be more contagious and deadly.
Who is at risk from coronavirus and flu?
People at high risk for developing complications from both viruses include:
- The elderly (65 years and older)
- People with underlying medical conditions such as heart and vascular disease, obesity, chronic lung and kidney disease, diabetes
- Anyone immunocompromised or taking a medication that lowers the normal immune response.
Additional risk factors that have disproportionately affected certain populations include Black, Indigenous, Latin, and other people of color; people with poor access to healthcare or are homeless; and people with disabilities.
Getting tested for the flu and coronavirus
There are several options available to people who would like to be tested for the flu or coronavirus.
The flu test is a nasal swab that results in several minutes and is widely available.
There are 2 types of testing for the SARS-COV-2 virus. The viral nasal swab test will tell you if you have the virus now. The antibody blood test will tell you if you had the virus in the past. There are multiple versions and availability of the viral tests.
At SignatureCare Emergency Center we offer the rapid antigen nasal swab test which results in 15 minutes, the molecular PCR nasal swab test which results in 2-7 days on average, and the antibody blood tests which result in 5-10 days. No test is 100% accurate, so following social distancing guidelines and wearing a mask remains a prudent mode of prevention.
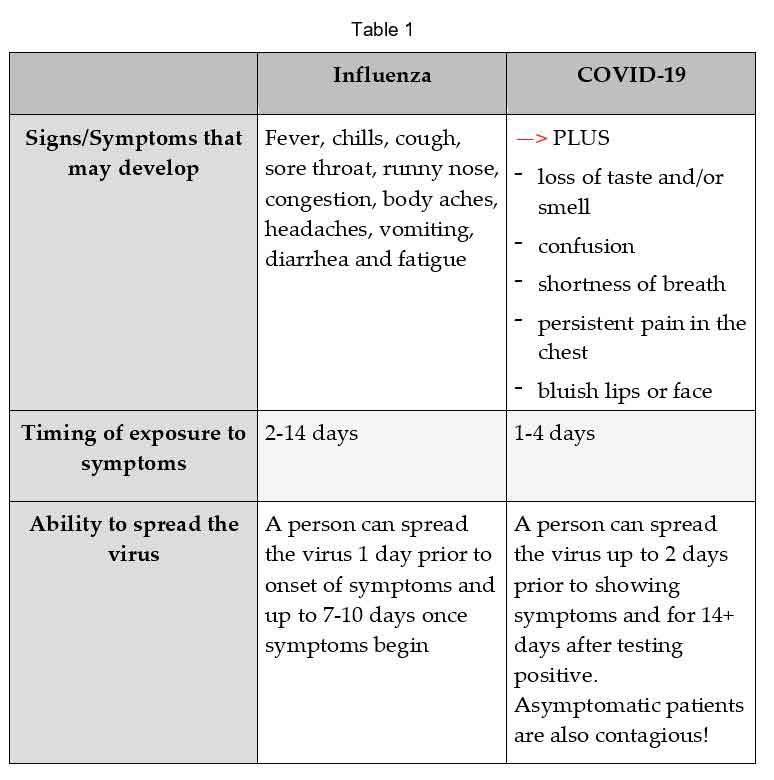
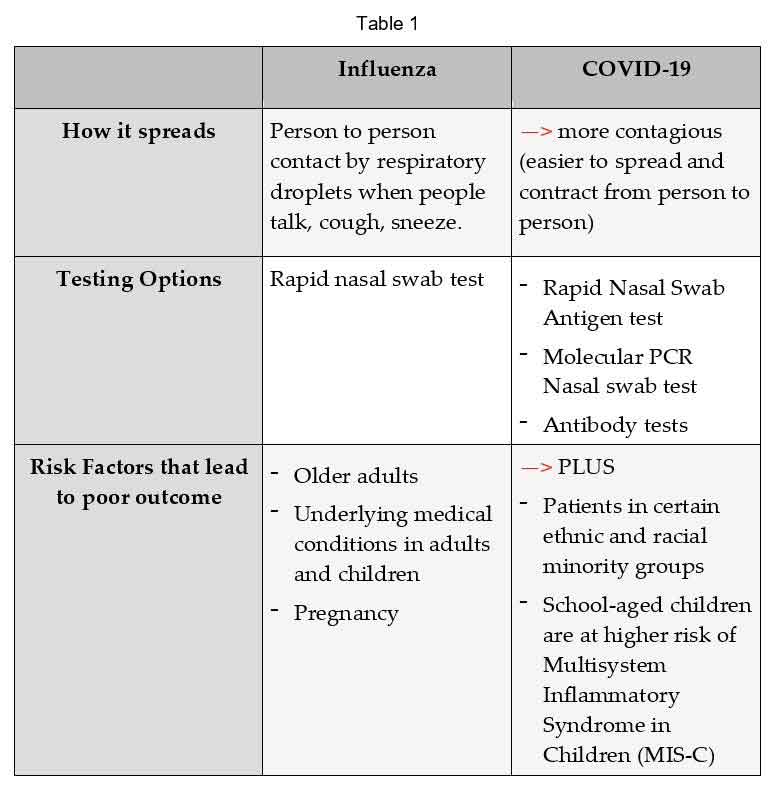
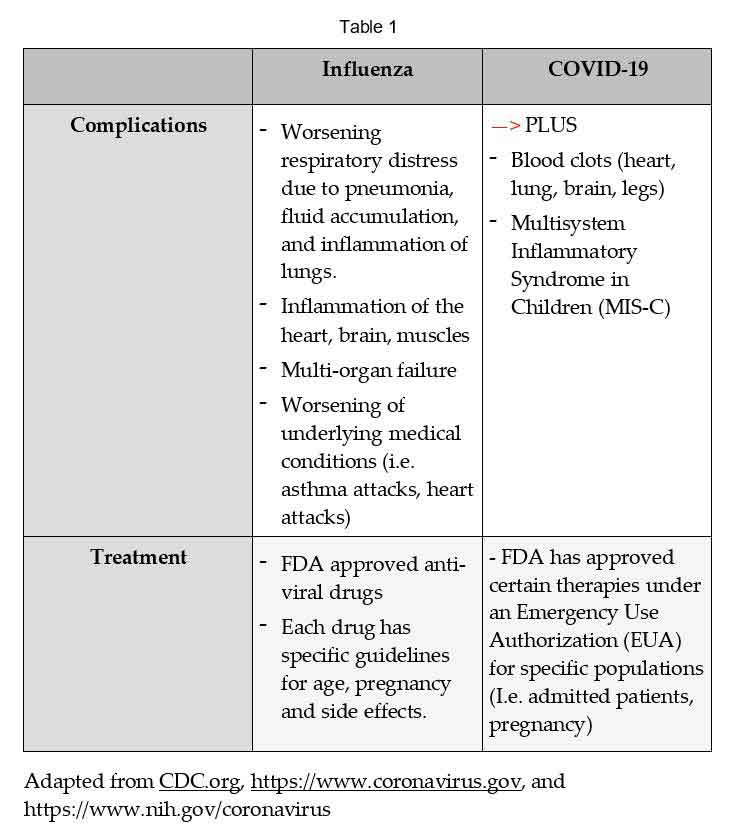
(Download pdf copy of this flu/coronavirus handy guide here).
How can I get prepared for the flu and coronavirus season?
1. Get vaccinated for the flu!
Currently, there is no FDA approved vaccine for coronavirus. There is one for the flu and is currently strongly encouraged! The CDC recommends all people 6 months and older to receive a flu vaccination. This includes pregnant women and people with chronic health conditions. There are various forms of the flu vaccine, so speak to your medical provider about which type is best suited for you. People who have a severe egg allergy or a history of Guillain Barre´ Syndrome (GBS) should not receive the flu vaccine. For a more in-depth explanation of vaccines, please visit https://www.cdc.gov/vaccines/.
The vaccine CANNOT cause the flu because it is an “inactivated” or killed form of the virus. Vaccines activate your immune system to make antibodies that recognize and eliminate the virus when you are re-exposed to it in the future. This allows your body to clear out the pathogen before it can cause illness. (https://www.publichealth.org/public-awareness/understanding-vaccines/vaccines-work/)
2. Social distance, Wear a mask, Wash your hands, Quarantine if sick

Viruses and bacteria are typically transmitted via respiratory droplets where they can be inhaled, touched, and subsequently ingested. They can also be transmitted via any mucosal barrier including the eyes and nose. We are still learning about the nature of transmission for the SARS-COV-2 virus so adhering to the basics will keep everyone safe.
– Wash hands for 20 seconds (sing happy birthday song)
– Stay 6 ft or more away from others
– Quarantine immediately if feeling ill
3. Manage your Stress and Strive for Restorative Sleep!

Several studies have shown that people with elevated levels of stress have a 3-4 times higher chance of catching a cold. Stress can lead to insomnia which can also hinder the immune system’s ability to respond to pathogens.
– Natural sleep aids such as melatonin, valerian root, magnesium, lavender, chamomile, passionflower extract, lemon balm, hops, and skullcap (always discuss options with your medical provider).
– Exercise: This can include both high and low-intensity activities.
– Anti-inflammatory diet: low in processed foods and sugar and rich in whole foods such as fruits, veggies, nuts, whole grains, and plant-based proteins and fish.
– Mind-Body: Meditation, tai chi, yoga, deep-breathing exercises, massage, guided imagery, walking, music, art, and spiritual practices are all amenable to daily practices that have incredibly positive impacts on your health.
– Stay connected with friends and family. Volunteer and help others.
Is There Anything I Can Take to Boost My Immune System?

Below are some vitamins and supplements that are considered generally safe and can help prime your immune system to fight off viruses.
Elderberry Extract 1 Tbsp 4X/day – Can reduce flu symptoms from 6 days to 2 days due to its potent antiviral effect on the flu viral proteins thus inhibiting the early stages of infection. Not recommended if you have contracted the SARS-COV 2 virus.
Melatonin 1mg at night – Anti-inflammatory activity
Vitamin D3 2000-4000 u/day – Has antiviral activity and deficiency is associated with worsening outcome if infected with SARS-COV-2
Vitamin C 500mg 2x/day – Anti-inflammatory and shortens duration and severity of common cold
Quercetin 250 mg/day – Found in onions and apples; anti-inflammatory activity
Zinc 15-30mg lozenges/day – (if dissolved in your mouth every couple hours, started within 24 hrs of symptom onset) can reduce symptoms and duration of upper respiratory infections.
Garlic, curcumin (Turmeric), green tea, and fish oil – anti-inflammatory and some antiviral activity.
I think I have the flu or coronavirus, Now what?

You are contagious, so quarantine and avoid others outside your household.
Several prescription medications exist for the Influenza virus, with the most common being Tamiflu®. If started within 48 hours of symptom onset, they can lessen the duration and severity of the illness.
All types of medications can be prescribed to children but may have age limitations. Most are safe in pregnancy but always consult with your doctor. Like all medications, there can be side effects, with nausea and vomiting being the most common. Your medical provider will discuss the risks versus the benefit of starting a flu medication.
There are no prescription antiviral medications for non-hospitalized patients available for the Coronavirus at this time. Until one is available or there is an effective vaccine, using the before-mentioned supplements (except Elderberry during active COVID-19 infections) along with the below options can help reduce symptom severity and progression.
Aspirin 81mg/day (if not contraindicated) – has anti-inflammatory effects and can reduce the prothrombotic effects of COVID-19.
Famotidine (Pepcid®) 20-40mg/day – reduces histamine release which may help reduce COVID-19 respiratory symptoms. Research is currently underway to investigate this off-label use.
Pulse Oximetry Monitoring – can help with identifying worsening symptoms and progression of the disease ( saturation dropping below 92%) and should prompt emergent evaluation.
Steam Hoods – 2-5 drops in a large bowl of hot water with a towel over your head is a natural way to relieve congestion and sinus pressure, especially if you cannot take a decongestant (history of hypertension, children). Use good quality essential oils of peppermint, eucalyptus, thyme, lavender. These oils can also be placed in a clean cool mist vaporizer.
When Should I Seek Medical Care?
Most cases of the common cold, flu, and coronavirus can be managed at home. However, people can get worsening symptoms requiring medical evaluation.
Seek medical care or Emergency Care when you feel profound fatigue, dizziness, worrisome pain, shortness of breath, or not comfortable managing symptoms at home.
Seek care if you are immunocompromised in any way or have a chronic medical condition in which the flu or coronavirus could worsen. If you would like to take an antiviral medication, you can make an appointment with your primary care provider or go to your local SignatureCare Emergency Center.
Bibliography
- CDC – cdc.gov/flu/index.htm
- Public Health – publichealth.org/public-awareness/understanding-vaccines/vaccines-work/
- Paul Marik, MD. Eastern Virginia Medical School Critical Care COVID-19 Management Protocol 09-24-2020. evms.edu/covidcare. Sept 24, 2020.
- Andrew Weil Center for Integrative Medicine. Integrative Approaches to COVID-19. https://integrativemedicine.arizona.edu/covid_19.html#strategies.
- Zakay-Rones Z et al. Inhibition of several strains of influenza virus in vitro and reduction of symptoms by an elderberry extract (Sambucus nigra L.) during an outbreak of influenza B Panama. J Altern Complement Med 1995 Winter;1(4):361-9
- Prasad AS et al. Duration of symptoms and plasma cytokine levels in patients with the common cold treated with zinc acetate. A randomized, double-blind, placebo-controlled trial. Ann Intern Med 2000 Aug 15;133(4):245
- Hemila H. Vitamin C supplementation and respiratory infections: a systematic review. Mil Med. 2004;169(11):90
Other Articles by Dr. Ruby Rose, MD –
Preparing for flu season
GERD (Heartburn) – Pain in the Upper Gut
Maximizing Wellness During a Pandemic

Dr. Ruby Rose, MD, is board certified in emergency medicine. Originally from New York City, Dr. Rose graduated from Vassar College in New York before obtaining her medical degree from Tufts University School of Medicine in Boston, Massachusetts. She completed her emergency medicine residency at University of Massachusetts. Dr. Rose has a passion for alternative care and recently graduated from the University of Arizona Integrative Medicine Fellowship in Tucson, Arizona. After relocating to Texas with her family, Dr. Rose worked in St. David’s Healthcare System where she served in several leadership positions. In her spare time, she enjoys watching her kids play various sports and riding her horse in the Texas Hill Country.









