Understanding High Blood Pressure and Hypertension Emergencies

Approved by Dr. Craig de WAAL
Medical Director – SignatureCare Emergency Center Austin, TX
ARTICLE SECTIONS
- What is Hypertension?
- Understanding Your Blood Pressure Numbers
- Risk Factors for Hypertension
- Signs and Symptoms of Hypertension
- When is High Blood Pressure an Emergency?
- Hypertensive Urgency
- Hypertensive Emergency
- What to Do if You Suspect a Hypertensive Crisis
- Our SignatureCare
What is Hypertension?
The American College of Cardiology and the American Heart Association define hypertension as a consistent measurement of your blood pressure 130/80 mm Hg or higher.
So, what does this mean?
It means that the force of your blood flowing through your blood vessels is too high and over time can cause damage to your organs.
If your primary care provider (PCP) suspects that you may have hypertension (high blood pressure), they will measure, record, and monitor your blood pressure numbers over time.
Your PCP may also ask you to monitor your blood pressure on your own using a “self-serve” machine or by using a home device to measure your blood pressure.
Some people become anxious at the doctor’s office and this anxiety can cause their blood pressure to artificially increase only at the doctor’s office. This is referred to as “White Coat Hypertension” and can cause you and your PCP to be unnecessarily concerned so it’s important to check your blood pressure outside of your doctor’s office if you suspect this may be the case.
To be diagnosed with hypertension, you should have 3 high blood pressure readings at 3 different times over a 6-month period.
SkiptheWaitBook an Appointment Today
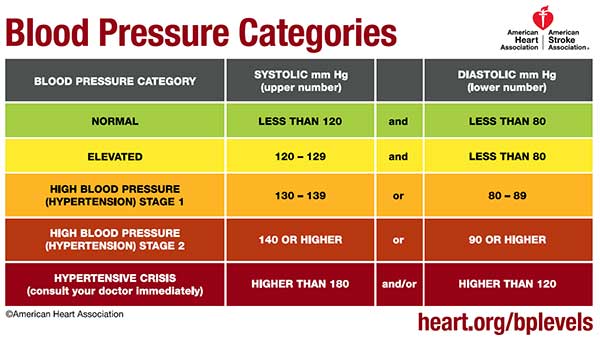
Understanding Your Blood Pressure Numbers
When you get your blood pressure (BP) taken, it is given as two numbers. For example, you might be told that your blood pressure is 120/80.
This number is always written as a fraction and refers to two things happening in your heart. The top number in the fraction is called the Systolic pressure (120/x). This number measures the highest blood pressure in your arteries when the heart muscle contracts.
The bottom number in the fraction is called the Diastolic pressure (x/80). This number measures the lowest blood pressure in your arteries when the heart is relaxed between beats. Both numbers are important in determining if your BP is normal or if you have hypertension.
Risk Factors for Hypertension
There are a number of factors that can put you at a greater risk for developing hypertension.
If you are aware of these risk factors and understand how they can affect you, you may be less likely to develop high blood pressure (HBP) or know you can help control it.
- Family History: If you have a close blood relative (especially parents or siblings) with HBP, you are at a greater risk of developing it yourself.
- Age: The older you get, the more likely you are to be diagnosed with HBP.
- Gender: Males are more likely to develop HBP before the age of 65. Women tend to develop hypertension over the age of 65.
- Race: More than 4 in 10 African-Americans suffer from high blood pressure. Hypertension in these individuals usually occurs earlier in life and is much more severe.
- Diabetes: More than 3 in 4 people with Diabetes are also diagnosed with Hypertension.
- Lifestyle: The choices you make can decrease your risk of developing hypertension. These factors include diet, exercise, being overweight and the use of alcohol and tobacco. The good news is that, unlike the others, these risk factors can be changed.
Signs and Symptoms
Many people may be surprised that they can have hypertension and not even know it. It is often referred to as the “silent killer” because high blood pressure typically does not have any apparent signs or symptoms.
Most of the damage to your body from high blood pressure takes place over a long period of time. However, some people do go on to develop emergencies related to blood pressure and may need urgent medical attention.
When is High Blood Pressure an Emergency?
The term hypertensive crisis is used to describe a quick and severe rise in blood pressure with measurements over 180/120 which can quickly lead to consequences like stroke, heart attack, kidney damage, loss of vision, or respiratory failure.
Unfortunately, some people have very difficult to control high blood pressures despite medication, so we need to consider what is a normal blood pressure for you as we decide what type of hypertensive crisis you are experiencing.
One type of hypertensive crisis is milder and can be treated conservatively as an outpatient. The other is very serious and requires immediate attention to prevent life-threatening complications.

Hypertensive Urgency
If your blood pressure is 180/120 or higher the first thing you should do is: Do Not Panic; wait about 5 minutes and check your blood pressure again.
If the repeat remains elevated, but you are not suffering from any symptoms like chest pain or shortness of breath, this is called Hypertensive Urgency and usually requires medication adjustment as an outpatient.
If you are not currently taking any high blood pressure medications, you may need to start them for any measured diastolic blood pressure of 110 mm Hg (x/110) or greater.
Hypertensive Emergency
If your blood pressure is 180/120 or higher AND you are experiencing symptoms that could be related to your high blood pressure you should go to the Emergency Room immediately.
Symptoms such as chest pain, shortness of breath, severe headache, changes in vision, difficulty speaking, dizziness, numbness/weakness, or even upper back pain all are potential symptoms of life-threatening high blood pressure.
When markedly elevated blood pressure is combined with these signs of organ damage, this is called Hypertensive Emergency and often requires admission to the hospital for immediate treatment.

What to do if You Suspect a Hypertensive Crisis
If you suspect that you or someone else is experiencing a hypertensive crisis, these are the steps that should be taken:
- Check your blood pressure.
- If your blood pressure is elevated to 180/120 or higher and you ARE NOT experiencing any severe symptoms, wait 5 minutes and take it again. Try to relax (easier said than done!) because anxiety can cause falsely elevated blood pressure readings.
- If the repeat BP measurement is the same or higher then you should seek medical attention. Call your Primary Care Provider first for instructions on medication adjustment and/or follow-up. If you cannot reach them, go to the Emergency Room.
- If your blood pressure is elevated to 180/120 or higher and you ARE experiencing warning symptoms (chest pain/upper back pain, shortness of breath, severe headache, dizziness, numbness/weakness, loss of vision, or difficulty speaking) then do not wait to recheck your blood pressure and instead you should go immediately to the Emergency Room for evaluation.
Our SignatureCare
At SignatureCare Emergency Centers we are ready 24/7 and 365 days a year to treat your emergency medical conditions. Our physicians are all Board Certified Emergency Physicians with years of experience treating all types of life-threatening problems, including Hypertensive Emergencies. Even if you’re not sure that you are having a Hypertensive Crisis, we welcome you to come in for a medical screening evaluation with a blood pressure check and to discuss your symptoms. Our luxury ER’s all have state-of-the-art technology with top-notch customer care and we are open 24 hours near you.




